The microbiome, trillions of microorganisms that intermingle with each person’s cells, influences human biology in ways we barely understand. Incorporating how it contributes to cancer development and prevention will lead to a more complete understanding of cancer.

Gut microbes
Credit: iStock
The microbes that crowd our guts, skin and respiratory tracts have a profound impact on how our bodies function in health and disease. The microbiome of trillions of bacteria, fungi and viruses intermingles with each person’s cells, influencing human biology in ways we have barely begun to understand. Incorporating the contribution of the microbiome to cancer development and prevention will lead to a more complete understanding of cancer and may shed light on strategies to halt or mitigate those contributions.
This complex community of microbes contains thousands of species and varies enormously from person to person. Its members protect us against pathogens, fine-tune our immune systems, shape how we use nutrients and produce a host of chemicals that impact the functions of our cells.
We have come to realize that the microbiome can also hasten or slow cancer development as well as influence our response to anticancer therapies. Manipulating this intricate ecosystem may one day help us prevent or treat cancer and other diseases.
Advanced genome technologies now make it possible to analyze microbial DNA to characterize communities that live in and on our bodies and how they relate to disease. We know that these communities are not stable because their members change as we alter our diets, spend time in new environments or take a course of antibiotics. Cancer, too, can affect the composition of a person’s microbiome. Efforts are underway to determine how factors such as inflammation, tumor development and progression and cancer therapy change a person’s microbiome.
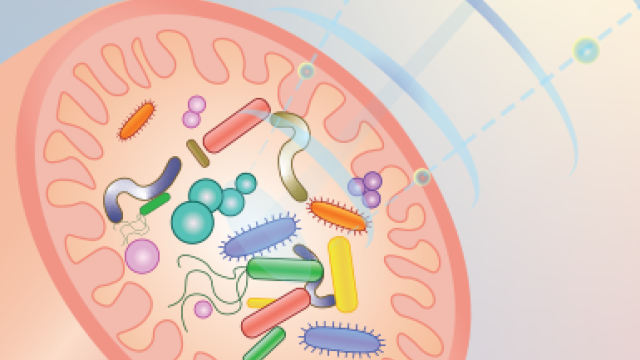
Scientists have learned that the microbiome, including the gut microbiome, can hasten or slow cancer development and influence responses to cancer treatment. Credit: iStock
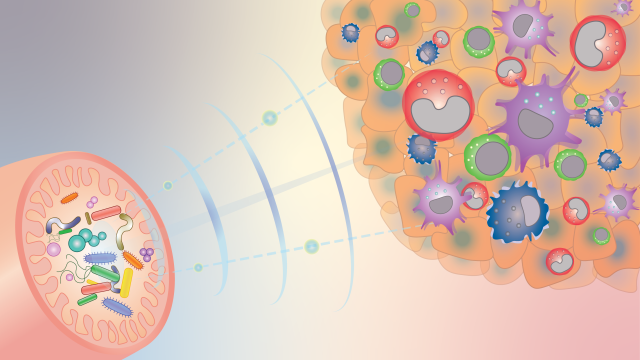
With new tools for molecular analysis, we can now extend our studies beyond surveying the microbiome and work toward a deeper understanding of what microbes do and how they interact with other cells. To gain a complete picture of the biological impact of these communities, it will be critical to investigate the genes present in different microbiomes and the vast range of chemicals that their members produce. Such studies will be complemented by work in animal models where investigators can carefully manipulate the composition of the microbiome to explore the mechanisms by which its members influence inflammation, immune activity and other processes. Another priority is to investigate the mechanisms that microbes and human cells use to communicate with one another. Once we understand how these communications work, it may be possible to interrupt or modify them to alter biologicial processes.
Maybe most importantly, a patient’s microbiome influences their response to cancer treatment. Researchers already know that a microbiome’s composition can modulate both the effectiveness of different therapies as well as their associated side effects. For example, certain types of immunotherapy work best when patients have highly diverse communities of gut microbes. Identifying ways in which the microbiome impacts the response to specific anticancer therapies will require extensive sequencing of microbial DNA and sophisticated bioinformatic analyses. Understanding these relationships is expected to help clinicians identify the best treatment for every patient and may also suggest ways we can modify individuals’ microbiomes to improve outcomes.
We cannot be certain of what we will find as we explore the relationship between cancer and the human microbiome. But elucidating its complexity is an immense opportunity that could uncover new aspects of cancer biology and find new ways to improve patient care.